Introduction: Why Understanding Keratoconus Matters for Eye Health
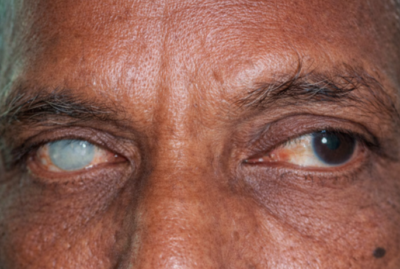
Keratoconus is a progressive corneal condition in which the cornea thins and gradually bulges into a cone shape. This irregular shape distorts vision, increases light sensitivity, and interferes with daily activities such as reading, driving, and screen use.
Improved awareness of keratoconus helps reduce delays in diagnosis and treatment. Early recognition, routine eye examinations, and access to evidence-based care play a critical role in protecting long-term visual health. Understanding the condition empowers individuals to recognise symptoms early, seek timely care, and manage progression effectively.
Understanding Keratoconus – Meaning & Key Facts
What Is Keratoconus?
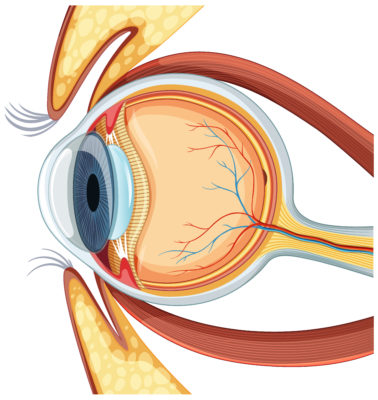
Keratoconus is a bilateral ectatic disorder marked by progressive corneal steepening and progressive corneal thinning. As the cornea weakens, it forms a cone-like protrusion that distorts the passage of light. It typically begins in adolescence or early adulthood and may worsen for several years before stabilising.
Although the exact cause is not fully understood, keratoconus is believed to result from a combination of genetic susceptibility and environmental factors. It remains one of the leading reasons for corneal transplantation worldwide, highlighting the importance of early diagnosis and intervention.
Symptoms and Signs to Watch For
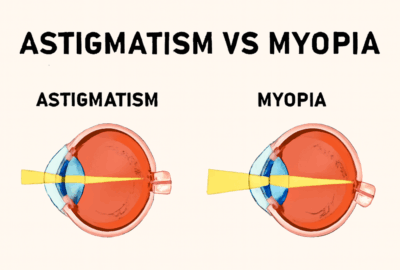
Common keratoconus symptoms include blurred or distorted vision, ghosting, halos around lights, difficulty seeing at night, light sensitivity, and eye irritation. Many patients struggle to achieve clear vision with normal glasses due to irregular astigmatism.
Individuals experiencing these symptoms should schedule an eye exam promptly, as early diagnosis supports more effective management. Recognising these signs of eye disease early can significantly improve outcomes.
Common Myths About Keratoconus – Separating Fact from Fiction
Myth – Keratoconus Causes Blindness
Fact: It does not cause complete blindness. However, untreated progression may result in severe vision loss. Appropriate treatment preserves vision.
Myth: Contact Lenses Can Prevent the Progression of Keratoconus
Fact: Contact lenses correct vision but do not stop progression. Poorly fitted lenses can worsen corneal damage. Specialised rigid gas-permeable, hybrid, or scleral lenses improve vision only.
Myth: Only Young People Develop Keratoconus
Fact: While commonly diagnosed before age 30, new cases may appear later in adulthood.
Myth: Keratoconus Has No Cure
Fact: There is no permanent cure, but effective keratoconus treatment options such as cross-linking or corneal transplantation can stabilise or restore vision.
Myth: Keratoconus Is Caused by Eye Rubbing
Fact: Chronic eye rubbing may accelerate thinning, but it is not the only cause. Genetics, UV exposure and allergies also contribute.
Myth: Keratoconus Affects Only One Eye
Fact: It usually affects both eyes, although progression may be uneven.
Myth: Correcting Your Vision Will Cure Keratoconus
Fact: Glasses and lenses manage visual distortion but do not stop the disease. Only medical procedures slow progression.
Can Keratoconus Be Prevented? Understanding Causes & Risk Factors
Keratoconus cannot be fully prevented due to its genetic basis. About 6% – 8% of cases report a positive family history. However, several risk factors for keratoconus may accelerate progression.
These include chronic eye rubbing, poorly fitted contact lenses, UV exposure, allergic eye disease and atopic conditions such as eczema. Conditions like Down syndrome and mitral valve prolapse are also associated. While complete prevention of keratoconus is not possible, reducing modifiable risks and ensuring early detection can make a significant difference.
Prevention & Management Strategies – Slowing Keratoconus Progression
Even though keratoconus cannot be entirely prevented, adopting protective habits helps slow progression:
- Avoid rubbing your eyes to prevent weakening of corneal collagen.
- Reduce UV exposure by wearing sunglasses with UV protection.
- Ensure contact lenses fit properly and follow specialist advice.
- Manage allergies to reduce itchiness and prevent rubbing.
- Schedule routine eye exams for timely intervention.
- Choose a balanced diet rich in antioxidants and maintain good hydration.
- Avoid smoking and take regular screen breaks to reduce eye strain.
Diagnosing Keratoconus Early – Screening & Tests
Early diagnosis is vital. Key diagnostic tests include corneal topography and tomography, which map the cornea’s shape and thickness in detail.
Slit-lamp examination helps evaluate irregularities or scarring. Regular screening for at-risk individuals promotes early detection of keratoconus, offering a greater opportunity for timely intervention, such as cross-linking, before significant progression.
Treatment Options – From Vision Correction to Surgical Solutions
Effective keratoconus treatment options depend on the severity of the condition:
- Glasses: Useful for early, mild cases.
- Rigid gas permeable, scleral or hybrid contact lenses: Improve visual quality by masking corneal irregularities.
- Corneal Cross-Linking (CXL): Uses riboflavin drops and UV light to strengthen the cornea and stabilise progression.
- Intrastromal Corneal Rings (Intacs): Flexible implants inserted into the cornea to reshape and improve stability.
- Corneal Transplant (Keratoplasty): Recommended for advanced disease where other measures no longer work.
Living with Keratoconus – Support & Coping Tips
Living with keratoconus often requires ongoing adaptation. Support groups, both online and offline, help individuals share experiences and coping strategies. Practical tips include using brighter lighting, adjusting screen settings, using high-contrast aids, and discussing workplace or academic adjustments when needed.
Psychological support can also be valuable, as fluctuating vision may affect confidence and daily comfort. Connecting with others who have keratoconus can provide reassurance and shared coping strategies.
Conclusion – Empower Yourself with Facts & Protect Your Vision
Keratoconus cannot be fully prevented, but early diagnosis, protective habits, and timely treatment significantly improve outcomes. Understanding myths, managing environmental triggers, and attending regular eye examinations support long-term visual stability.
Informed decisions, guided by professional care, allow individuals with keratoconus to maintain vision, independence, and quality of life.