Many patients walk into the clinic convinced they have “just irritation,” only to discover they actually have bacterial conjunctivitis and need treatment. People ignore redness for days, parents assume a child has a dust allergy, and contact-lens users continue wearing lenses despite discharge. These small mistakes allow the infection to spread quickly.

What is Bacterial Conjunctivitis?
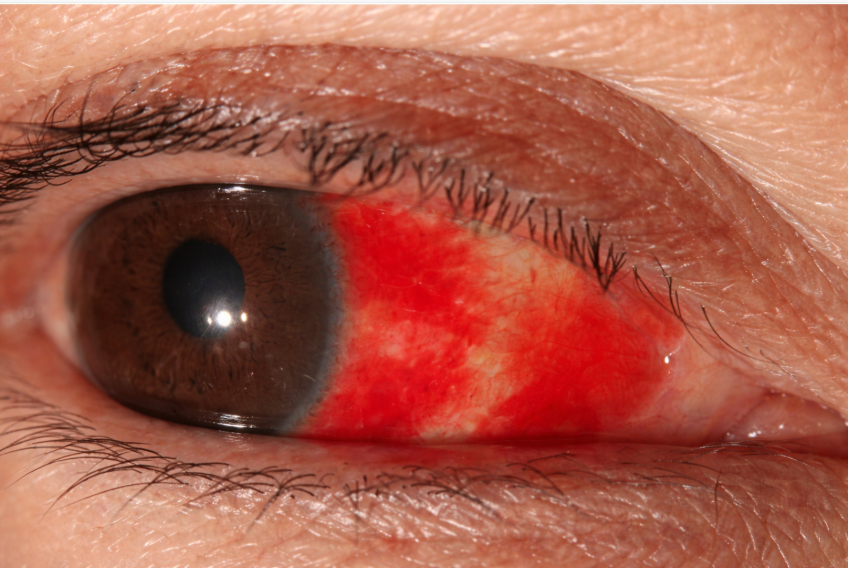
Bacterial conjunctivitis is an infection of the conjunctival tissue, the thin membrane covering the white of the eye and the inner eyelids, caused by bacteria such as Staphylococcus, Streptococcus, or Haemophilus. These organisms naturally live on skin and surfaces, which explains why simple hand-to-eye contact can trigger infection.
Unlike allergic conjunctivitis, bacterial infection produces thick discharge and crusting around the eyelids. Many patients wake up with eyelids stuck together in the morning. This symptom alone often signals bacterial involvement.
Bacterial infections, however, generate sticky mucus or pus-like discharge. Doctors choose the best treatment for bacterial conjunctivitis based on severity, patient age, and medical history. Early intervention prevents complications and shortens recovery time.
Risk Factors for Bacterial Conjunctivitis
Several everyday habits increase the likelihood of infection. Common risk factors include:
- Poor hand hygiene: Touching eyes after contacting contaminated surfaces
- Improper contact lens care: Sleeping with lenses or reusing solution
- Sharing personal items: Towels, eye makeup, or pillowcases
- Recent respiratory infections: Bacteria from the nasal passages are spreading to the eyes
- Chronic eyelid inflammation: Conditions like blepharitis
Certain medical conditions also increase susceptibility:
- Diabetes
- Weak immune system
- Sinus infections
- Chronic allergies
Understanding these triggers helps patients adopt preventive habits alongside proper treatment for bacterial conjunctivitis in adults and children.
Symptoms and Diagnosis of Bacterial Conjunctivitis
Symptoms usually appear suddenly and worsen within a day or two. Many patients first notice mild redness before discharge becomes obvious. Common symptoms include:
- Redness in one or both eyes
- Thick yellow or green discharge
- Eyelids sticking together, especially in the morning
- Irritation or gritty sensation
- Mild blurred vision caused by mucus
During clinical examination, ophthalmologists evaluate several indicators:
- Conjunctival redness pattern
- Type and quantity of discharge
- Eyelid swelling
- Corneal clarity
Signs of Bacterial Conjunctivitis
Certain clinical signs strongly indicate bacterial infection rather than viral or allergic conditions.
Doctors often look for:
- Yellow or green discharge that returns after wiping
- Eyelid crusting that causes sticking after sleep
- Localised redness beginning in one eye
- Mild eyelid swelling
- Irritation without severe pain
Patients sometimes misinterpret early symptoms and delay care. Early recognition of these signs allows quicker bacterial conjunctivitis treatment, reducing contagious spread.
Diagnostic Procedures for Bacterial Conjunctivitis
Most diagnoses occur through a clinical examination conducted by an ophthalmologist.
Typical diagnostic steps include:
- Visual inspection of the eye to evaluate redness and discharge
- Slit-lamp examination to assess the conjunctiva, cornea, and eyelids
- Assessment of corneal clarity to rule out deeper infection
- Review of medical history and symptoms
In complicated cases, doctors may recommend additional tests such as:
- Conjunctival swab culture to identify resistant bacteria
- Tear duct evaluation if recurrent infections occur
- Fluorescein staining to check corneal integrity
Differential Diagnosis of Bacterial Conjunctivitis
Several eye conditions can resemble bacterial conjunctivitis, leading to confusion among patients. Doctors usually differentiate between:
- Viral conjunctivitis: Watery discharge and highly contagious
- Allergic conjunctivitis: Intense itching and watery eyes
- Blepharitis: Inflammation along the eyelid margin
- Dry eye syndrome: Irritation and burning without thick discharge
- Corneal infection: More severe pain and vision disturbance
Correct diagnosis ensures patients receive the best treatment for bacterial conjunctivitis rather than inappropriate medication.
Managing Bacterial Conjunctivitis
General Treatment and Hygiene Recommendations
- Proper hygiene: Patients must wash their hands frequently and avoid touching their eyes unnecessarily.
- Warm compresses help loosen crusted discharge: Patients should gently clean eyelids using sterile cotton or a clean cloth soaked in warm water.
- Bacterial conjunctivitis home treatment: Warm compresses and eyelid cleaning help relieve symptoms, but they cannot replace medical therapy in moderate or severe infections.
- Prevent cross-contamination: Avoid sharing towels, cosmetics, or eye drops during the infection period.
- Cosmetic safety and replacement: Replace eye makeup after recovery to prevent reinfection.
Medical Therapy: Antibiotic Eye Drops and Ointments
Doctors commonly prescribe eye drops for bacterial conjunctivitis treatment. These medications eliminate bacteria and reduce inflammation. Antibiotic drops usually require application several times daily for about five to seven days. In more severe cases, doctors may add antibiotic ointments at night.
Patients frequently stop medication once redness improves. This habit often causes relapse. Completing the prescribed course ensures bacteria do not survive and reappear. Contact lens users must discontinue lenses immediately during treatment. Continued lens wear prolongs infection and increases the risk of corneal complications.
Medical follow-up
Follow-up visits ensure proper healing. Doctors reassess the eye after a few days if symptoms fail to improve. Persistent redness, pain, or blurred vision may indicate corneal involvement or resistant bacteria.
In such cases, doctors modify medication or conduct additional testing. Patients with recurring infections may require evaluation for eyelid disorders, sinus infection, or systemic disease. While conjunctivitis rarely requires eye surgery, ophthalmologists occasionally perform minor procedures if blocked tear ducts contribute to repeated infections.
Conclusion
Bacterial conjunctivitis remains one of the most common eye infections encountered in clinical practice. Most cases resolve quickly when patients receive early diagnosis and proper treatment. Simple habits such as washing hands, avoiding eye rubbing, and following prescribed medication make a significant difference in recovery.
Ignoring symptoms or relying solely on self-treatment often prolongs the infection and increases the risk of spreading it to family members or colleagues. If redness, discharge, or eyelid crusting persists beyond a day or two, a professional evaluation ensures safe and effective treatment for bacterial conjunctivitis while protecting long-term eye health.