Key Takeaways
- Penetrating Keratoplasty (PKP) is a surgical operation to replace a diseased cornea with a donor cornea to restore vision.
- PKP is applied in conditions like keratoconus, corneal scarring, dystrophies, degenerations, and edema.
- Complete preoperative evaluation and rigorous donor cornea screening are crucial for a successful operation.
- The procedure entails the removal of the deformed cornea and the insertion of a donor cornea, with sutures to hold it.
- Postoperative care includes medication and follow-up to prevent rejection of the graft.
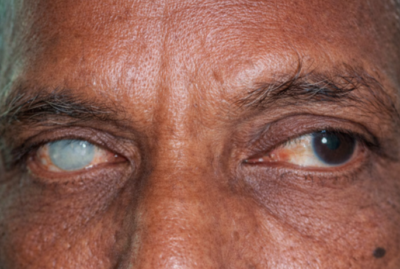
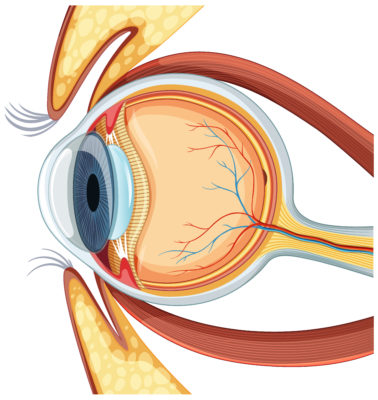
Penetrating Keratoplasty (PKP), commonly known as corneal transplant surgery, is a surgical procedure designed to restore vision by replacing a damaged or diseased cornea with a healthy donor cornea. The cornea is the transparent front part of the eye responsible for focusing light onto the retina. When the cornea is compromised due to injuries, infections, or degenerative conditions, vision can be significantly impaired, necessitating surgical intervention.
Indications for PKP
PKP is recommended for a variety of corneal conditions that cannot be effectively managed with other treatment modalities. Some common indications include:
- Keratoconus: A progressive thinning and bulging of the cornea, leading to distorted vision.
- Corneal Scarring: Resulting from injuries, infections, or previous surgeries.
- Corneal Dystrophies: Inherited conditions causing abnormal deposits in the cornea.
- Corneal Degenerations: Age-related changes affecting the cornea.
- Corneal Edema: Swelling of the cornea due to endothelial dysfunction.
Preoperative Evaluation
Before undergoing PKP, a thorough preoperative evaluation is essential to assess the patient’s overall health and suitability for the surgery. This includes a detailed medical history, comprehensive eye examination, and various diagnostic tests such as corneal topography, pachymetry, and endothelial cell count. The information gathered during this evaluation helps the surgeon plan the surgery and determine the appropriate donor cornea.
Donor Cornea Selection
The success of PKP depends on the availability of a healthy donor cornea. Donor corneas are obtained from eye banks, where they undergo meticulous screening and preservation processes. Factors such as tissue compatibility, size, and overall quality are carefully considered to ensure a successful transplantation. The use of advanced imaging technologies has improved the precision of donor tissue matching.
Surgical Procedure
PKP is typically performed as an outpatient procedure under local or general anesthesia. The surgical steps include:
- Removal of the Diseased Cornea: Using specialised instruments, the surgeon removes the central portion of the patient’s damaged cornea, creating a circular opening.
- Donor Cornea Placement: The healthy donor cornea, prepared to match the size and shape of the recipient’s cornea, is then sutured into place using fine stitches. In some cases, newer techniques such as Descemet’s Stripping Automated Endothelial Keratoplasty (DSAEK) or Descemet’s Membrane Endothelial Keratoplasty (DMEK) may be employed for selective replacement of specific corneal layers.
- Suturing: Sutures are carefully placed to secure the donor cornea in position. These sutures may be absorbable or non-absorbable, and their removal is often a gradual process over several months.
Postoperative Care
Following PKP, patients require diligent postoperative care to promote healing and reduce the risk of complications. Medications, including antibiotics and anti-inflammatory drugs, are prescribed to prevent infection and control inflammation. Regular follow-up visits are scheduled to monitor the healing process, assess visual acuity, and adjust medications as needed.
Complications and Challenges
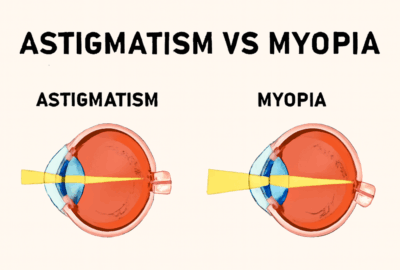
While PKP has a high success rate, complications may arise, including graft rejection, infection, and astigmatism. Graft rejection, where the recipient’s immune system attacks the donor cornea, is a serious concern and requires prompt intervention.
Penetrating Keratoplasty remains a valuable and effective procedure for restoring vision in individuals with various corneal disorders. Advances in surgical techniques, donor tissue processing, and postoperative care have significantly improved outcomes. As technology continues to advance, the field of corneal transplantation is likely to witness further innovations, offering even better results and enhancing the quality of life for those in need of vision restoration. Patients considering PKP should consult with their ophthalmologist to determine the most suitable treatment plan based on their individual circumstances.