Glaucoma is a non-contagious eye disease that requires continuous medication to control intraocular pressure and preserve vision. The medical management of glaucoma is based on effective glaucoma medications.
Patients and clinicians should understand the types, mechanisms, and appropriate applications of these drugs. This is an information guide on how glaucoma is medically treated, its roles and advantages, and the probable side effects of glaucoma medications.
What is Glaucoma?
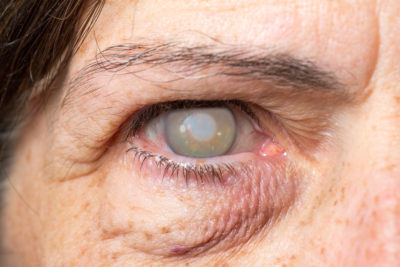
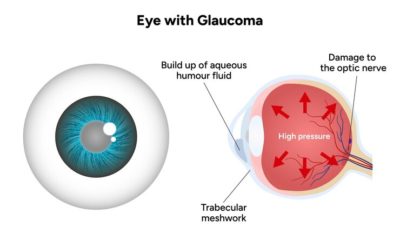
Glaucoma is an eye disease characterised by progressive damage to the optic nerve and typically accompanied by high intraocular pressure (IOP). It is one of the leading causes of permanent blindness worldwide.
The medical definition of glaucoma focuses on optic neuropathy, characterised by a loss of visual field. Early diagnosis and medical management of glaucoma are critical to prevent vision loss, which underscores the importance of regular eye pressure testing and ongoing monitoring.
Medical Management of Glaucoma
The main aim of medical management of glaucoma is to reduce IOP, as the single risk factor that is adjustable and has been shown to slow glaucoma progression. Treatment of glaucoma commonly begins with topical eye drops aimed at decreasing or accelerating the production of aqueous humour or promoting its drainage.
Drugs may either be administered alone or in combination, depending on the severity of the disease and response. In combination with medication, frequent follow-up of glaucoma provides therapeutic efficacy and keeps side effects in check.
Types of Glaucoma Medications
Prostaglandin Analogues
They are normally the first-line treatment for open-angle glaucoma, as they are effective in increasing aqueous humour outflow through the uveoscleral pathway. Common drugs include latanoprost, bimatoprost and travoprost. The most frequent side effects of these glaucoma medications are mild redness of the eyes and alterations.
Beta Blockers
The beta blockers, like timol drops, lower intraocular pressure by reducing the production of aqueous humour. They are commonly used as second-line agents or as substitutes if prostaglandins are inappropriate. Systemic side effects of beta blockers can include fatigue or bradycardia, which should be taken into consideration in the medical history.
Alpha Agonists
Brimonidine, an alpha-2 adrenergic agonist, reduces IOP by reducing fluid secretion and enhancing outflow. They are usually administered twice or thrice a day and may lead to the development of mild stinging, redness, and fatigue.
Carbonic Anhydrase Inhibitors
These decrease the secretion of aqueous humour in the eye. They are especially helpful in patients not responding adequately to first-line therapies. Some may experience temporary stinging or a bitter taste after application.
Rho Kinase Inhibitors
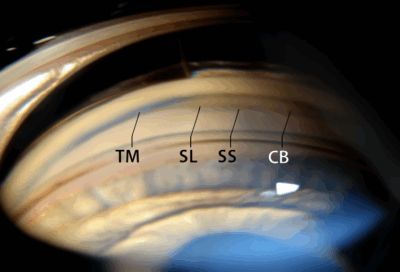
The newer glaucoma medications, like netarsudil, improve aqueous humour drainage through the trabecular meshwork. These drops can cause mild redness or irritation initially, but are highly effective in patients who are unresponsive to traditional drugs.
Combination Eye Drops
Combination drops contain two different active ingredients, reducing the need for multiple bottles and improving patient compliance. Examples include timolol with dorzolamide or latanoprost with timolol.
Glaucoma Medication Side Effects
Common Local Side Effects (Redness, Burning)
Glaucoma medications, in particular, prostaglandin analogues and carbonic anhydrase inhibitors, often result in eye irritation, redness, and burning sensations. The effects are mild and short-lived, but may influence patient compliance when persistent.
Systemic Side Effects to Watch For
Some of the systemic effects of beta blockers include slowed heart rate or respiratory symptoms. Alpha-agonists may cause dry mouth or drowsiness, and systemic carbonic anhydrase inhibitors may cause tingling and gastrointestinal upset. Close observation is necessary during routine glaucoma check-ups.
Managing Side Effects Effectively
If the side effects of glaucoma medication become troublesome, doctors may adjust the dosage or switch to another class. Using punctal occlusion (gently pressing the inner corner of the eye after applying drops) can minimise systemic absorption. Regular glaucoma follow-up visits help monitor pressure control and side effect management effectively.
Tips for Taking Glaucoma Medications Correctly
- Wash your hands thoroughly before applying drops.
- Tilt the head back, pull down the lower lid, and apply one drop into the pocket.
- Close the eye gently and press the corner near the nose for 1-2 minutes to enhance absorption.
- Follow the prescribed schedule; skipping doses can affect pressure control.
- Store eye drops as instructed; some may need refrigeration.
- Never stop or change medication without consulting your ophthalmologist.
Next Steps in Glaucoma Treatment: Beyond Medications
When eye drops fail to achieve the target pressure, laser therapy or surgery may be necessary.
Signs That You May Need Laser or Surgery
Worsening visual fields, uncontrolled IOP despite maximal medical therapy, or intolerance to drugs may signal the need for interventions. These interventions can include selective laser trabeculoplasty or trabeculectomy to maintain eye health.
Conclusion
Glaucoma medications play a pivotal role in managing this potentially sight-threatening condition. Understanding different drug types, mechanisms, and side effects helps optimise treatment outcomes. Patient education on proper use and adherence, combined with regular glaucoma follow-up and eye pressure examination, is critical in preserving vision for a lifetime.