Key Takeaways
- Some people are more likely to develop problems in the cornea based on their genes, previous infection, or injury.
- Prolonged periods of increased eye pressure can weaken the cornea, and risks for cataract surgery are present.
- Smaller eyes and complex cataracts complicate the surgery and risk to the cornea.
- Proper surgical technique and post-op care can save a delicate cornea.
- DSEK and DMEK, two sophisticated cornea transplants, can restore vision in severe conditions.
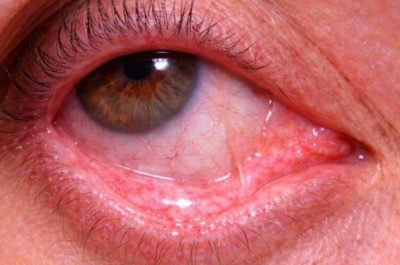
Mrs. Fernandes was in deep agony and she could not understand why she has a weak cornea. According to her, all her friends have undergone cataract surgery and none of them were told that they have a weak cornea and that there is a risk of corneal swelling after the cataract surgery. I wish it was so simple and all human bodies were alike. Some of us are born with a higher predisposition for certain diseases like increased risk of cornea failure and swelling.
Some of the common reasons for a weak cornea-
- Genetic predisposition– Inherent inborn disease like Fuch’s Endothelial Dystrophy, Posterior Polymorphous Dystrophy etc increase the risk of corneal swelling in the later years of life. This risk is magnified whenever any extra stress is imposed on the corneal endothelium like any injury, a complicated eye surgery, eye inflammation or increased eye pressure. In these cases it is important to plan the cataract surgery at the right time and with correct set of precautions and surgical modifications.
- Previous corneal infections– Previous endothelial infections like viral endothelialitis can make the corneal endothelium weaker. This in turn increases the risk of corneal failure either due to recurrent nature of these infections or often precipitated by any eye surgery.
- Corneal Injury– Severe blunt or penetrating injuries can cause substantial harm to cornea and induce a significant corneal weakness. Cataract surgery in these eyes can sometimes initiate severe non-resolving corneal edema.
- Prolonged episodes of high eye pressure– Increased eye pressure over a long period can make the corneal endothelial cells weak. These cells have very little reserve capacity left. Cataract surgery in these eyes can occasionally predispose to corneal edema.
Besides these conditions some other eye conditions predispose to corneal edema after cataract due to other reasons-
- Structurally smaller eyes– These eyes have very little space in the front part of the eyes. Any surgical manipulation is not just challenging but can also be more injurious for the corneal endothelium.
- Complicated cataracts– These cataracts are not like normal age related cataracts. These cataracts have associated features which can require more surgical manipulation leading greater surgical trauma, can lead to higher risk of more inflammation and higher eye pressure postoperatively.
Steps needed to manage the cases where cornea is weak before cataract surgery and there is a greater risk of corneal edema-
- Modification of surgical technique– It is essential that in these cases less of phaco energy is used during the procedure and more chopping is done. But at the same time the movement inside the eye should be less. Basically a gentle surgery and profuse use of special viscoelastics which coat and protect the corneal endothelium.
- Prevent and treat any post-surgery inflammation– After the cataract surgery it is important to reduce and treat any inflammation that may occur due to the surgery or the pre-existing condition.
- Treat any high eye pressure– increased pressure in the eye after cataract surgery can be more damaging to the already weak cornea. It is therefore imperative to take aggressive steps to control the eye pressure and bring it back to normal.
- Treat any surgical complications– Flat anterior chamber, lens touching the endothelium, vitreous touching the cornea, areas of large descemets detachment etc. All these conditions require immediate attention.
Overall I think performing cataract surgery begins with first recognition and identification of these cases, planning the cataract surgery at a stage when cataract is not too hard and it can be performed without the use of too much phaco energy, counselling the patient, taking appropriate steps to protect corneal endothelium during the surgery, ensuring uneventful postoperative period by controlling inflammation and eye pressure.
In spite of all these precautions many a times some of the patients due to severe stage of their corneal weakness may progress to develop irreversible corneal edema. These cases then need corneal transplantation. However good news is that now we have many advanced types of cornea transplantation which does not require transplantation of entire cornea and no stitches are given. Procedures like DSEK and DMEK have revolutionized the way we perform cornea transplantation in these cases of corneal edema. One of my close friends aunt came to me with an irreversible corneal edema after her cataract surgery. She was deeply troubled as she could not see after cataract surgery, and had accompanied pain and watering as well. She was highly depressed and couldn’t understand why she has these problems even when her cataract surgeon was one of the known experts. After her eye check-up I re-assured her and informed her of the advanced corneal disease called Fuch’s Endothelial Dystrophy” in her eyes. We performed a type of cornea transplantation called DSEK for her and this restored her vision to normal.